
With a Limb Difference, Forrest Is Perfect in His Own Way
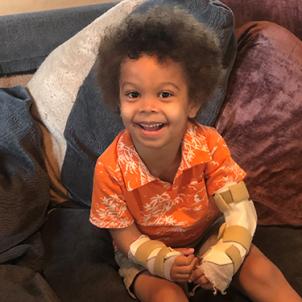
Like many kids his age, Forrest is a bundle of energy. The 6-year-old loves to play with his friends, run around the house and get on the floor to wrestle. You would never guess he has a limb difference that affects both of his arms and hands.
Forrest was born with a pattern of symptoms related to thrombocytopenia-absent radius (TAR) syndrome, a rare disorder that can impact multiple parts of the body, but most notably the blood and skeletal systems. In Forrest’s case, the condition affected his forearms, specifically the radius bone, which did not develop at all and led to the ulna bone growing with a curve. As a result, his hands remained in a curled-up fetal position after birth.
“That was the first indication something was different,” recalls Forrest’s mom, Nivla. “This wasn’t found in utero, so we were very surprised, and there were a lot of questions and worries about what to do next and how to care for him.”
At the time of Forrest’s birth, doctors ran multiple tests to figure out what he had, but the results didn’t yield a definitive diagnosis. Nivla and Forrest’s father, Devon, left the hospital after five days with a handful of referrals, including one for Children’s Hospital Los Angeles. There, they met Nina Lightdale-Miric, MD, Director of the Hand and Upper Extremity Orthopedic Program in the Jackie and Gene Autry Orthopedic Center, who immediately identified the condition as TAR.
“It was the first time we heard someone put a pin on it right away and say, ‘Yes, I’ve seen this before and I am a specialist who works with children just like Forrest and have so much to tell you,’” says Nivla.
A comprehensive care team

Unlike other limb differences, TAR syndrome is actually a blood-born condition that can cause anemia or a low platelet count—and in severe cases can be fatal. A physical difference, whether in the arm, wrist or hand, is just one of the symptoms.
“When I teach and train student surgeons, I tell them how hand surgery can save lives, and one example is being able to recognize TAR,” says Dr. Lightdale-Miric. “If you can see the typical pattern in the limb difference, you can immediately get a family in touch with a hematologist and that can save their child’s life so they don’t run out of platelets.”
Fortunately for Forrest, TAR syndrome was not life-threatening if he received treatment. Dr. Lightdale-Miric reached out to colleagues in the Cancer and Blood Disease Institute and Division of Medical Genetics at CHLA to create a comprehensive care team that could address all of Forrest’s needs. A hematologist checked his platelet levels, a geneticist conducted tests to get more answers, Dr. Lightdale-Miric assessed the surgical options, and occupational therapists were on standby to assist with braces for his wrists.
“It’s just one of the wonderful ways we work together as medical teams here at Children’s Hospital,” Dr. Lightdale-Miric says about the multidisciplinary aspect of treating patients with complex conditions.
Living life more freely
Because of the varying nature of TAR syndrome—some children can have missing, weaker or bent thumbs or fingers, while others have stronger digits—there is no one-size-fits-all treatment. Instead, each case is discussed in depth with parents or caregivers to find the best option for their child. That can include surgeries to reposition the wrist and arms, nonsurgical interventions such as splints, casts and braces, or a combination of both.

“Parents will often ask me, ‘How do I know what my newborn wants? What if they don’t like what we chose for them when they were young?’ And that is something we work through together,” says Dr. Lightdale-Miric.
“If I’m directly asked, I will give my opinion, and I like to introduce them to families who decided to go through with surgery and others who decided not to,” she adds. “We also share the incredible research we’ve done at Children’s Hospital, which found that the brain is incredibly plastic and that children will eventually learn to use their hands and fingers in whatever form they’re in.”
Without the radius bone, the ulna bone in the arm tends to grow a little curved, like the letter C, and the thumb points inward toward the chest, affecting a child’s dexterity and mobility. Forrest’s treatment started with casting and splinting, with great results, before moving onto a series of surgeries from the time he was 21 months old to the most recent one in 2021.
For the first surgery, Dr. Lightdale-Miric and Attending Physician Milan Stevanovic, MD, reset the ulna bone and performed subsequent surgeries to straighten the wrist by inserting rods. When the rods slipped out of place—“as Forrest has gotten older we’ve learned he is definitely an active kid,” says Nivla—a follow-up to reinsert them held up in his right hand, but not in the left yet. Consistent splinting with occupational therapy, however, has helped make the curvature of the left arm less limiting and has allowed Forrest to access his world more freely.
Now in the first grade, Forrest loves reading, math and watching the big kids play different sports during recess. He came home the first week of school and enthusiastically told his mom he wanted to learn how to play tetherball and volleyball.
Forrest’s future
Forrest comes to the Autry Orthopedic Center every few months so that orthopedic specialists can check his growth spurts and maintain the position of his hands and arms, while occupational therapists adjust his braces as needed. Once he has outgrown the rod in his right arm and finishes growing altogether, Dr. Lightdale-Miric will have a conversation with Forrest about the future.
“He is not broken or missing anything. Forrest is perfect in his own way, and there are options such as surgeries and therapies that may make his arm, hand and thumb function longer or stronger,” says Dr. Lightdale-Miric. “So we’ll talk about what I call ‘your arms for life’: the arms he’ll take for his driver’s permit and license, the ones he’ll head off to college with, the arms he’ll have if he one day has children, and whether they’re functional enough or if he wants to explore further options.”
It’s a big decision he’ll have to make once he’s older, but for now, Forrest simply enjoys coming to CHLA and seeing the care team that has treated him since he was 1 month old.
“It’s set up in a way that he knows the hospital setting isn’t intimidating or this scary experience, but rather everyone there wants to help and support him,” says Nivla. “It’s a great outlook to have for someone who’s probably going to have plenty of interactions with doctors over his lifetime.”
‘Bigger-picture view’
The Hand and Upper Extremity Orthopedic Program at CHLA treats more than 300 patients like Forrest every month. From congenital limb differences and brachial plexus to acute flaccid myelitis and cleft hand, the team specializes in all types of disorders using a holistic approach to care. A dedicated psychologist helps families navigate decisions about surgery and patients to feel confident, while the Center for Achievement of Teens and Children With Hand Differences (CATCH) Program gives kids the opportunity to connect with others and strengthen their resilience.
Dr. Lightdale-Miric established CATCH in 2011 as an extension of how she views every patient: beyond the physical difference to who they are as unique individuals.
“I had wonderful mentors who taught me to look up from the hand and to take in the needs of the entire child,” she says. “I think to be a good surgeon you have to consider your whole patient, not solely the condition itself.”
That viewpoint has been particularly impactful for Forrest’s parents, from the time they first walked into Children’s Hospital Los Angeles to today.
“When we’ve been so focused on, ‘How do we fix this?’ Dr. Lightdale-Miric has helped us take a bigger-picture view that sees each child as more than just their diagnosis but who they are as a whole person,” says Nivla. “I have really appreciated that perspective.”
“Our worries about Forrest are so different than what they were in the first month of his life,” she adds. “We’re so grateful for the care that we’ve received.”


