Part 2: ‘We Knew It Must Be Done’
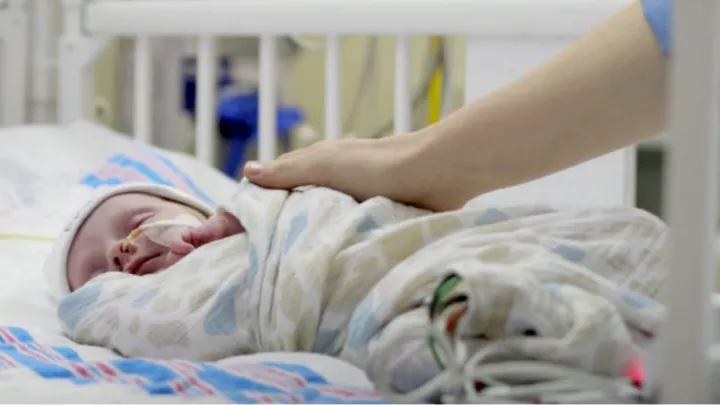
In the concluding half of this two-part story, a CHLA family learns whether their home survived the Woolsey fire, baby Max’s cleft lip is repaired, and Max’s mother tries to sort through the aftereffects of 10 days of trauma. (Read Part 1.)
Lauren’s experience with Malibu fires went back to November 1993, three months after she moved into the region. They tended to succumb quickly, so presuming the Woolsey fire, as it had been named, would do the same, she didn’t pack for a long evacuation. She had an emergency checklist stashed, but the moment overwhelmed her and she never got to it.

“I couldn’t find it that morning,” she says, “and I just couldn’t think. I couldn’t think. I just thought, ‘Forget it. Let’s get in the car and go.’ I was wearing the same thing every day, washing the clothes overnight.”
With their son, Max, at Children’s Hospital Los Angeles, in the Steven & Alexandra Cohen Foundation Newborn and Infant Critical Care Unit, his third intensive care unit in four days, Lauren and her husband had to track down somewhere to stay each night as the roads to their Malibu neighborhood stood closed. In eight nights the family moved five times, trading off between hotel rooms and friends’ homes.
Though Malibu was shut off, the situation in Thousand Oaks began to settle and the local hospital reopened, ending Max’s stay at CHLA after two days. He would have to be in intensive care for several more weeks, and Lauren returned him to Thousand Oaks because of the facility’s proximity to her home, Max’s pediatrician and her older daughter’s school.
She found the helicopter back from CHLA more serene than the initial flight the opposite way, but sobering. She could see how much of the Conejo Valley had burned, and that the fire was still active in Malibu Canyon. On three occasions, based on updates she was getting from her Pepperdine University office, she thought the fire would consume her home. Ultimately the house was spared, and on Nov. 17 Lauren received word her family could return to it. The worst of the damage in Malibu occurred further north.
“That’s our story pretty much,” she says.
Defying the rule of 10s
Well, no, not in full. That just gets you to intermission. Leave now and you don’t learn what became of Max, who remained in the hospital for another 2 ½ weeks, getting treated for several conditions related to his prematurity. When his health normalized he was released Dec. 5, only weeks before his scheduled cleft lip surgery in January.
William Magee, MD, DDS, a surgeon in CHLA’s Division of Plastic and Maxillofacial Surgery, wanted to operate on Max at 6 weeks old, counting out from what would have been the completion of a 40-week pregnancy term. That would go against the convention begun in the 1960s called the “rule of 10s,” which holds that children with clefts should be treated when they are at least 10 weeks, weigh at least 10 pounds, and have a hemoglobin level of at least 10 grams.
Dr. Magee says the two surgeons who conceived the rule had no research behind it. “Didn’t have any facts or stats. And ironically, in 2019, the entire world still thinks that that’s the right age to take care of clefts—with no data.”
Favorable surgical outcomes have fed the theory, but that’s more coincidental than scientific, Dr. Magee believes. The science argues for repairing clefts sooner, he says, to take advantage of the mother’s estrogen, which remains in a baby's system through the first six weeks of life and is crucial to cartilage formation. At CHLA, with his partner, Jeffrey Hammoudeh, MD, DDS, Dr. Magee has done more than 100 cleft repairs on infants within six weeks of birth to take advantage of the estrogen presence.
“We knew it must be done,” Lauren says. “We didn’t mind Max having a cleft lip. We loved him and loved the way he looked and we’d have been perfectly fine if things had remained the same, but we knew he couldn’t go through life like that. We knew that was not best for him.”
A modicum of Malibu
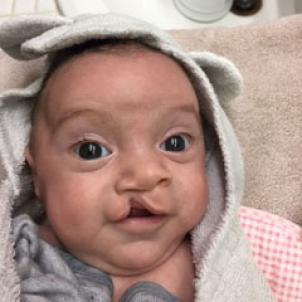
Max’s case was ordinary, a unilateral cleft that split the right side of his lip. What was out of the ordinary was the family’s profile, which Dr. Magee saw would undercut a stereotype about cleft lips and who suffers them.
“When we think of clefts,” he says, “we think of all these kids who are out there in the middle of a poor town in the Philippines or in the middle of Africa or Southeast Asia, because Operation Smile and other organizations have telecast it that way.”
Max’s circumstances disassemble that notion. Lauren and her husband are upper middle class and live in Malibu—though Lauren wants to undo another stereotype: “We’re not typical celebrity Malibu or Malibu Colony Malibu.” Whatever degree of Malibu they are still places them well apart from the impoverished families generally associated with clefts.
While Lauren’s advanced age at pregnancy (43) is among the risk factors, it’s just as possible that Max’s cleft lip and palate happened accidentally. Dr. Magee explains that clefts result from some defective balance of genetics and environment, and though he runs the world’s largest study on the topic, having gathered the DNA of 16,000 affected families, the research hasn’t yet been able to say why.
“The human face is made like a puzzle,” he says. “It fuses together in different pieces in the first trimester of gestation. It’s remarkable that all those events typically work out normally, but 1 in 800 times they don't. And it can’t always be predicted. Does prematurity play a role? What’s going on in utero? Is it the mom? Is it the dad? Is it the environment? Is it the gene? Is it random? We don’t know.”

Max’s surgery was done in mid-January. Dr. Magee has a before-and-after that illustrates the procedure’s success. He zipped up Max’s cleft and left hardly any trace of a zipper behind. In a few years he will go back in and smooth over the residual bit of roughness on the gum to ensure Max’s teeth come in normally. A second surgery to close the cleft palate will be done soon after Max turns 1 in October.
And sometime after that, or before if she can set herself to the task, Lauren wants to write down everything that occurred during the family’s merciless 10-day crucible last November—the Borderline shooting, the five moves in eight nights, her anxious drive across the canyon hounded by flames as if she were trying to outrun Armageddon. The entire series of trials and calamities might have seemed concocted for a Navy SEAL drill, but unfortunately made for the grimmest nonfiction.
As for her own before-and-after, Lauren says she hasn’t gotten to it yet. “It will take a long time to unpack it all and have it settle. I didn’t have a chance to ruminate on it as it was happening because we were in survival mode.”
What sort of imprint was left? The most that can be said for now is that unlike her son, she’ll wear hers on the inside.