Facial Paralysis Care Program
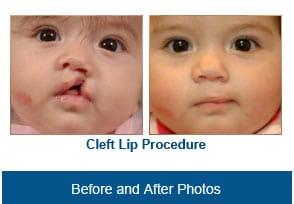
The Facial Paralysis Care Program in the Division of Plastic and Maxillofacial Surgery offers the latest surgical techniques, including transplantation of nerves and muscles to the face to provide movement.
Types of Facial Paralysis
Congential Facial Paralysis
Most children with congenital facial paralysis (present at birth) are affected only on one side of the face (unilateral facial paralysis). Fewer children have facial paralysis on both sides of the face, which is called bilateral facial paralysis.
Acquired Facial Paralysis
In acquired facial paralysis, the facial muscles or nerve stop functioning normally at some point in infancy or early childhood. Most often, this is due to an injury to the facial nerve. However, there may be other causes such as tumors, infections and rare diseases.
In Moebius Syndrome (or Möbius Syndrome), children have a congenital, permanent, severe, and usually bilateral facial paralysis. Moebius Syndrome involves not only the seventh cranial nerve (the facial nerve), but also the sixth cranial nerve, which controls outward eye movement. Other nerves may also be involved, including the glossopharyngeal (the ninth cranial nerve) and vagus nerves (also known as the tenth cranial nerve, responsible for the gag reflex), and the hypoglossal nerve (also known as the twelfth cranial nerve, responsible for tongue movement). Because of the inability to express emotions and difficulties with speech, children with Moebius Syndrome may be incorrectly categorized as learning disabled. Other physical differences may be present, all of which may be addressed at Children's Hospital Los Angeles.
Moebius Syndrome Resources
Bell's Palsy is a common, acquired, unilateral facial paralysis that can affect all age groups. Children develop Bell's Palsy most commonly after a viral infection. The facial paralysis usually resolves on its own over time.
Common Problems Associated with Facial Paralysis
Depending on the severity, children with facial paralysis may demonstrate various problems. Many have trouble with drooling and keeping food and liquid in the mouth. Pronouncing certain words and letters may be difficult because of the inability to close the lips properly. Children with acquired unilateral facial paralysis require special care to protect the cornea (outermost layer of the eye). In this situation, the ability to close the affected eye may be disrupted, which can result in damage from drying out.
The social consequences of severe facial paralysis are particularly problematic. Unable to smile or frown, these children cannot communicate on an emotional level with their family and friends. Children may develop poor self-esteem from being teased or misunderstood by their peers, ultimately leading to social isolation. Family and patient counseling may alleviate some of these problems.
Treatments for Facial Paralysis
Several options are available to treat a child with facial paralysis. A thorough examination and determination of severity can be performed at the Facial Paralysis Center at our hospital. At the first visit, the possibility of surgery to improve function will be discussed. Two surgical procedures are currently available to create a smile, sometimes referred to as facial reanimation surgery. One procedure is called a cross-facial nerve graft and the other is a free functional muscle transplant.
Both of these surgeries are long and technically demanding, and they require hospitalization for a short recovery period. In addition to these surgical procedures, your child may need assessment and treatment by other members of the health care team.
Occupational therapists, speech pathologists, social workers and nurses are available to work with you and your child around such issues as learning how to maximize your child's facial muscular function, speech development, and the development of social and emotional coping mechanisms. The treatment programs are individualized to each child’s specific functional needs.
Facial Paralysis or Facial Reanimation Surgery
The specific details of your child’s surgery will be discussed upon initial consultation with the surgeon in the Facial Paralysis Center. Below are general guidelines.
Surgery for Unilateral Facial Paralysis
Cross-Facial Nerve Graft
The cross-facial nerve graft is designed for children who have unilateral (or one-sided) facial paralysis. A long nerve in the leg called the sural nerve, is removed. The nerve itself is expendable, producing an inconsequential small patch of sensory loss to the side of the foot. It is used as a nerve graft to transfer impulses from the non-paralyzed to the paralyzed side of the face. The sural nerve is attached to the facial nerve and is then tunneled under the skin of the face to the paralyzed side. A small incision is made in front of the ear, extending slightly along the lower jawline. This allows the surgeon to locate the nerves, attach them to the nerve graft, and place them in the proper position. The final scar is well-hidden and has the appearance of a facelift scar. The small incisions on the leg are closed with dissolvable sutures, similar to closure of the facial incision. There may be several small scars or possibly one long scar on the back of the leg below the knee where the sural nerve is harvested.
After Cross-Facial Nerve Graft Surgery
After surgery, children are hospitalized for about three or four days until they are eating and walking normally. Over the next several months, the motor fibers from the functioning facial nerve will grow into the nerve graft. In approximately six to 12 months, sufficient regeneration of the nerve will have occurred, and the child will then be ready for the second stage of the operation, a free functional muscle transplant.
Free Functional Muscle Transplant
In the free functional muscle transplant, a small piece of an inner thigh muscle, called the gracilis muscle, is removed and transferred to the paralyzed side of the face. This muscle is most frequently used for several reasons:
- It has its own separate blood and nerve supply.
- The portion of muscle that is used nicely approximates the force needed to generate an elevation of the corner of the mouth.
- Only a small scar remains along the upper part of the inner thigh, which is easily concealed.
- Taking the muscle from the inner thigh does not result in any functional deficit or difficulty walking.
An incision is made along the front of the ear in the face and extends for a short distance underneath the lower jawline. This allows the surgeon to see the blood vessels and nerves in the face. Great care is taken to position the muscle and anchor it in the area around the corner of the mouth. The blood vessels and nerves of the muscle are connected to the blood vessels and nerves in the face under high-power magnification. The incision on the face mirrors the scar from the cross-facial nerve graft. This is usually well-hidden. The incision on the inner thigh is also closed with dissolvable sutures.
After Free Functional Muscle Transplant Surgery
After surgery, children remain in the hospital for about one week. Only soft foods are allowed for about two weeks. It is important that no caffeine be consumed under any circumstance. On discharge, you will be expected to supervise your child’s activity closely at home. No sports activities are allowed for two or three months. Several months are required for the muscle to regain its function. When it does begin to contract on demand from the normal side, it will provide two very important functions. First, by elevating the lower lip and corner of the mouth, the muscle will assist in improving speech. Second, by the same action, the child will be able to generate a smile. The resulting smile will never be perfectly symmetrical, but the improvement will allow for a less noticeable difference. The free functional muscle transplant is by far the most effective procedure currently available for facial paralysis reconstruction.
Surgery for Bilateral Facial Paralysis
Children with bilateral facial paralysis will require the free functional muscle transplant surgery to be performed on each side of the face. There is no need to perform a cross-facial nerve graft. This is because there are no working facial nerves to use. The gracilis muscle from the inner thigh is used. See Surgery for Unilateral Facial Paralysis for a detailed description.
The difference in the application of the free functional muscle transplant for bilateral facial paralysis centers on the nerve supply used to stimulate the muscle. In these cases, the nerve of the muscle is connected to a nerve that supplies one of the muscles used for biting and chewing (the masseteric branch of the trigeminal nerve). Once again, this nerve branch is expendable and results in no discernible effect on chewing.
Questions About Surgery
Day of Surgery
Upon arrival to the hospital, you will be directed to the preoperative area where you will be checked in by our staff. You will meet the anesthesia team who will perform a physical exam, verify the clinical history and explain the procedure for undergoing general anesthesia. After a final preoperative visit by your surgeon, the nurse will bring your child to the operating room. Depending on the particular surgery being performed, he or she will be in the operating room from four to 10 hours.
After Surgery
After surgery, you will be taken to the recovery room to join your child. A short observation period in the recovery room will be followed by transfer up to your child's hospital room. Expect to be in the hospital for five or more days. Assistance with hotel arrangements may be provided, if you are traveling from outside the greater Los Angeles area. Your child will eat and drink a soft diet as soon as he or she wants. Getting out of bed the day after surgery is encouraged, but with plenty of assistance to prevent falls. Medication to minimize pain and discomfort will be provided. Recovery is usually uneventful and proceeds without difficulty.
There may be some swelling and bruising from where the nerves and muscles are removed, but this is usually well-treated with pain medication. There will also be swelling and bruising in the face. This will likely persist for two or more weeks. A mouth guard is used to splint the corner of the mouth and protect the transplanted muscle while it heals. This mouth splint will remain in place for 10 days, but can be removed periodically for cleaning and eating purposes. Appointments to see your surgeon will be made following surgery.
Smile Timeline
As early as three months after surgery, children will begin to feel twitching in the new muscle. At this point, facial muscle exercises should be practiced several times each day in front of a mirror.
For children with unilateral facial paralysis and who have undergone cross-facial nerve graft followed by a free functional muscle transplant, simultaneous movements on both sides of the face will begin. In this case, the muscle transplant is attached to the working facial nerve in the non-paralyzed side, and a smile is created automatically when the non-paralyzed side activates.
Children who have had the muscle transplant procedure on both sides must learn to activate their new smile by biting down or clenching the teeth together. With practice, children learn to do this easily, although the smile is never completely spontaneous.
Watch: Kiana Deane, Patient Story Featured on ABC News
Before and After Photos
Before Surgery
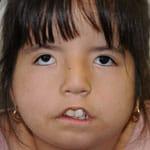
Preoperative at Rest
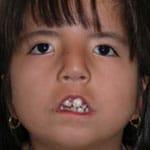
Preoperative Maximal Smile
After Surgery
Post-Op Maximal Smile


