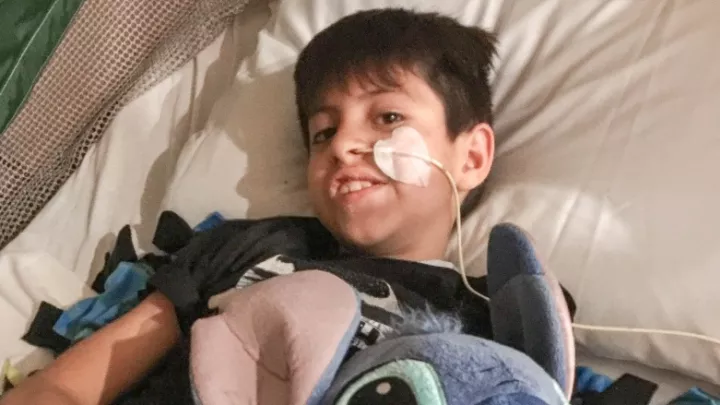
Caiden Moran’s Chance to Hear
When Caiden Moran was born, he failed the newborn hearing screening, a standard test given to all babies before they leave the hospital. So his parents brought him back for a recheck. And he failed again.
Caiden, it turned out, was born with underdeveloped cochleae and cochlear nerves, which transmit sound from the ear canal to the brain. As a result, he was completely deaf, and cochlear implants, which bypass damaged portions of the ear and transmit sound directly to the cochlear nerve, weren’t an option.
Children born with congenital deafness like Caiden’s have never heard a sound in their lives—not their parents’ voices, or the sound of birds chirping, or the blast of a safety siren.
“I was sad,” says Caiden’s father, Tommy Moran, a U.S. Navy submarine fire control technician stationed in Hawaii. “I didn’t know anybody who was deaf, and I didn’t know sign language. I didn’t know how to be a good dad and raise a deaf child.”
A whisper of hope
Just a decade ago, children like Caiden had no chance of ever hearing. Today, auditory brain stem implantation can open their worlds to sound.
The expanding field of functional neurosurgery treats malfunctions of the central nervous system caused by congenital abnormalities, trauma or seizures through the implantation of electrodes or the placement of therapeutic lesions. The auditory brain stem implant (ABI) is just one example of this type of therapy. With the ABI device, electrodes are implanted on the brain stem, sidestepping the ear altogether. An external microphone and transmitter convert sound to electrical signals and send them directly to the brain stem.
“The new idea for the auditory brain stem implant is to take children who have never heard anything, whose brains aren’t even designed to receive hearing because they were born without cochlear nerves,” says Mark Krieger, MD, chief of medical staff and head of the Division of Neurosurgery, and inaugural holder of the Billy and Audrey L. Wilder Endowed Chair in Neurosurgery at Children’s Hospital Los Angeles. “You’re not actually putting a sound into the brain,” says Krieger. “You’re coming up with an electrical stimulation pattern that the brain can perceive as hearing.”
Learning to hear
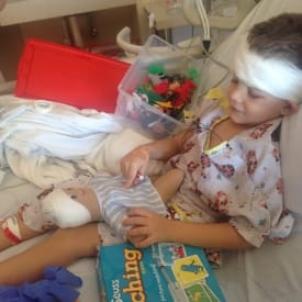
Meanwhile, Caiden’s family had adjusted to their new reality. They connected with the deaf community and also learned sign language, figuring that this would be Caiden’s main method of communication for life. Then Caiden’s mom, Danielle, heard about a new clinical trial—the first ABI study in the U.S. supported by both the Food and Drug Administration and the National Institutes of Health—of which Krieger was a co-investigator for CHLA. The five-year trial is following patients between 2 and 5 years old to test both the safety of the treatment and its efficacy in allowing deaf children to hear.
In January 2015, Krieger performed the surgery, attaching electrodes to Caiden’s brain stem. Caiden was only a month shy of his fifth birthday, just sneaking under the study’s upper age limit.
“The brain has circuits in place to learn how to talk, smell, hear, etc. But if there’s no input, these circuits tend to fade away,” says Krieger, who is also co-director of the Neurological Institute at CHLA and professor of Neurological Surgery at the Keck School of Medicine of the University of Southern California. “You lose that hard wiring at age 5 or 6, so you can’t do this procedure on older kids.”
A year and a half later, Caiden is showing signs of progress—which is no small feat. Caiden must not only learn to hear, but also what to do with this new information. His mother remembers the first time they activated his device.
“I wasn’t sure how he was going to react, but he was just surprised. It didn’t scare him, so that was good,” says Danielle.
“They have to learn how to make use of that information and understand that when they hear a person talking, it’s a human speaking,” says Amy Martinez, clinical research coordinator for the ABI study. “They have to learn how to make sense of these sounds and understand that these are syllables, these are parts of speech, and so on and so forth.”
Caiden still primarily communicates by sign language, but he has started using a handful of words, and also recognizes the backing-up beep of the school bus when it picks him up for first grade. He goes to two different kinds of speech therapy, three times a week.

“In general, we’re not seeing really great leaps in progress until about three years post-activation,” says Martinez. Yet she thinks Caiden’s got a good chance for success. “He’s a motivated, bright child, and he seems to be able to take in the auditory information.”
Krieger agrees. “He is such a social kid; he’s highly motivated to interact.”
Martinez remembers an anecdote Caiden’s mom shared. “There was a little girl that he was friends with who had a cochlear implant, and he was so excited that he was going to have a device that, at least on the outside, looked like hers,” she says.
“He’s gone a lot farther; way more than I expected,” says Danielle. “We’re just proud of Caiden, because he has worked so hard.”
How you can help
To help kids just like Aiden, consider making a donation to Children's Hospital Los Angeles. Visit CHLA.org/Donate.