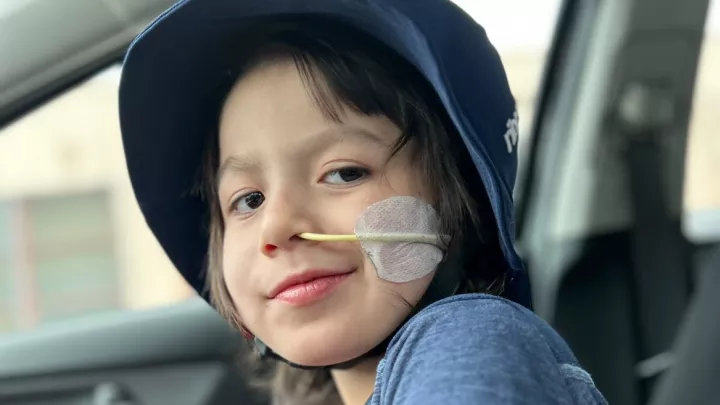
Can a New Way to Treat a Tumor Help Kai Beat Brain Cancer?
Melissa found Children’s Hospital Los Angeles in July 2021, when she was on a frenzied search for help for her infant son.
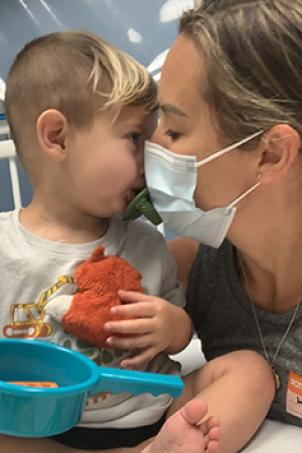
Five months earlier, Kai had been diagnosed with atypical teratoid rhabdoid tumor, known as ATRT, an especially menacing brain cancer with a bleak prognosis. The doctors who made the diagnosis after removing the tumor recommended that Melissa and her husband, Chasen, not intervene with treatment.
“We ran from them as fast as we could,” Melissa says. But where to? Searching out an alternative opinion was an immense effort. “Nobody said, ‘This is how we treat it, this is what we’re going to do,’ because there’s no real protocol for ATRT.”
The family moved east, picking up stakes from San Jose, California, to pursue treatment, but after four months of chemotherapy, Kai relapsed just before his first birthday. The cancer reappeared in the same area of Kai’s brain, along with more, smaller lumps nearby and on his spine. The medical team told the family that there was no answer for recurrent ATRT and discontinued Kai’s care.
Again facing a desperate scramble to find an expert who would treat Kai, Melissa contacted doctors across the country, but got nowhere until a pediatric oncologist in Texas listened to her story and thought of a colleague. She told Melissa, simply, “Call Dr. Margol.”
A new way of attacking a tumor
One of the few physicians with expertise in ATRT, Children’s Hospital Los Angeles oncologist Ashley Margol, MD, Director of the hospital’s Brain Tumor Center, administers a treatment protocol called MEMMAT developed specifically to target recurrences of the most destructive pediatric cancers, including atypical teratoid rhabdoid tumor.
Melissa says she didn’t hold back. “We emailed her, we called her. She called us back and said, ‘Get on a flight. I’ll see him in a couple of days.’”

How fast was the response? The time elapsed between the date Dr. Margol received the email and the date the family was in her office was five days.
“We were completely overwhelmed,” Melissa says. “We had no idea this even existed, this possibility. We were thinking we were only going to have a certain amount of time with our kid. And then we were presented with a little bit of hope, which was—no, you can’t describe that.”
The acronym MEMMAT is a merger of recurrent medulloblastoma, ependymoma and ATRT. It’s what’s called an antiangiogenic therapy, which means it is designed to prevent new tumors from forming by cutting off their blood supply, as opposed to standard chemotherapy, which kills active cancer cells.
“I’ll give you an example,” Dr. Margol says. “If I have a plant and I start depriving it of water, that's one way of killing it, right? Versus if I pulled the plant out of the dirt and chopped it into 10 pieces. We know that tumors, unless they have their own blood supply, can’t grow. Eventually they wither away and die. So it’s kind of a different way of attacking a tumor.
“Honestly,” she says, “there’s no standard of care for relapsed ATRT. There’s really no standard of care for upfront ATRT. It’s such a rare disease. There are only about 50 kids in the U.S. every year who are diagnosed with it.”
‘Fifty percent doesn’t mean anything’

What separates MEMMAT from conventional chemotherapy is the delivery of medicine, which goes directly into the fluid surrounding the brain through a small catheter called an Ommaya reservoir. That’s a potential advantage over the standard intravenous injection of chemotherapy, which can run up against a protective screen called the blood-brain barrier and be kept from reaching cancer cells in the brain and spine.
The therapy knocked out the several new, smaller tumors Kai presented with at CHLA, while the recurrent large tumor was removed by neurosurgeon Mark Krieger, MD, Surgical Director of the Brain Tumor Center, who holds the Billy and Audrey L. Wilder Chair in Neurosurgery. Multiple rounds of radiation followed. Last October, with repeated MRIs showing no evidence of cancer and seeing no benefit to be gained from more chemotherapy, Dr. Margol advised ending the treatment to spare Kai any further side effects. The most recent scan in January was also clear.
“Dr. Margol and the MEMMAT protocol absolutely saved Kai,” Melissa says.
However, Dr. Margol has had frank talks with the family about the chances of surviving the disease. MEMMAT is not seen as a cure, she says. It can extend and improve life, but recurrent ATRT remains a nearly insurmountable cancer.
“I don’t go over statistics because children are not statistics,” Dr. Margol says. “Fifty percent doesn’t mean anything, right? Your kid is 100%. So I don’t have that conversation. There is never a scenario where I tell someone, ‘I’m sorry, there’s nothing I can do.’
“I do tell every family, ‘My goal is to cure your child, and I’m going to do everything I can to make that happen.’ My goal is always for the family to understand that we’re on the same team from the get-go. I don’t know how the journey’s going to end, but we’re all on this train together.”
An ellipsis that signals hope
Each clean MRI report offers some relief, but hardly enough time to exhale before the next one. As each scan draws closer Melissa gets a swell of “scanxiety,” as parents of pediatric cancer patients call their nervousness before an impending test and the wait for the outcome.

“About a week leading up to MRIs, we’re irritable, we’re scared, we’re worried, we’re all the things, but we still have to function,” Melissa says. She asks her husband to check the patient portal for the results. “I can’t open the app. He does it because I just sit and shake until we know we’re in the clear for another little while.”
That’s just one of the ways Chasen has held Melissa together. She says that Kai’s 6-year-old brother, Cruz, also provides support. “It’s a family fight,” she says. “I’m only a small part of the reason we’re still upright each day.”
Kai turns 3 in July. He gets physical and occupational therapy to address the weaknesses related to his disease and treatment, including walking and talking. A stroke he suffered after his initial brain surgery impaired the right side of his face, which makes eating a challenge.
“I don’t think of them as deficits at all,” Melissa says. “I think of Kai as thriving based on what he’s been through. He’s the sassiest 2-year-old you’ve ever met in your whole life. He’s been telling us every day that he wants to go to preschool. We’re like, ‘OK, well, let’s try to get you potty-trained and we’ll take that next step,’ because he seems to be ready.”
Dr. Margol told the family that if Kai gets to two years with no appearance of cancer, then she will be comfortable saying his prognosis has improved meaningfully. Yet seeing in her notes that he has passed the one-year mark draws a small inflection of optimism. “Oh yeah, look at that,” she says.
“I told the family, ‘It’s still a very small possibility that we can cure him, but we’re certainly going to try.’ To be honest, I didn’t think we would be in this space right now where he doesn’t have any tumor, but ...” In the upturn of her voice as it trails off, in all the open-ended qualifiers, in certainly, but, and small possibility, is a slender allowance of hope.
“I don’t know that I think about whether there’s going to be a cure,” Melissa says. “I live in survival mode, truthfully. I want to be hopeful. I’m just really cautious about how optimistic I am. The reality is that ATRT is a beast and can come back at any time. So it’s scan to scan. I’ll take it all day long because I didn’t think I would get the opportunity to experience such a beautiful kid, and I’m getting that. I’m grateful for it.”