
After Suffering From Long COVID, Lucas Wants to Help Others
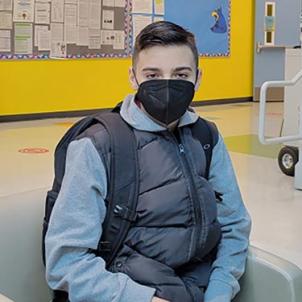
It was supposed to be a normal school day morning: Eat some breakfast, grab the backpack and head out the door. But on Aug. 16, 2021—just three days into the new school year—Lucas could only muster a few words.
“Dad, I feel sick. I think I’m going to throw up,” the high school sophomore said to his father, Robert, before rushing to the restroom.
A trip to a local urgent care center revealed Lucas had COVID-19. But unlike those diagnosed with the disease who typically recover within two to four weeks, Lucas’ symptoms progressively worsened. First came the headaches, then severe fatigue, followed by extreme sensitivity to light and what seemed like never-ending nausea.
“It was bad,” recalls Robert. “He had no strength to get out of bed. We had a bucket ready for him in case he couldn’t make it to the bathroom. He was so weak.”
Lucas was one of the approximately 5 to 15% of children and teens infected with SARS-CoV-2 who develop long COVID.
The condition can cause patients to struggle for months with lingering, often debilitating symptoms. For Lucas, the headaches were so intense that it affected everything from his eating to sleeping. He wasn’t able to return to school.
“I remember thinking, ‘Is this ever going to end?’” says the 15-year-old. “I was genuinely terrified.”
A holistic approach
Long COVID caught Lucas and his parents by surprise. He had received both doses of the COVID vaccine, and a year earlier he experienced his first bout of COVID, which passed quickly and felt like the common cold.
This time, however, “he was just a different kid—unrecognizable,” says Robert. “To see Lucas, a usually healthy kid without any underlying issues, that was hard.”

Lucas’s pediatrician referred the family to Children’s Hospital Los Angeles, one of the few institutions in California offering long COVID recovery care for pediatric patients. The clinic is led by physicians from the Division of Infectious Diseases who first evaluate children, then coordinate care with specialists from other areas of the hospital, such as cardiology, sleep medicine and neurology.
“This is a disease that a single physician cannot manage because the symptoms are so varied,” says Sindhu Mohandas, MD, a pediatric infectious disease expert and Attending Physician at CHLA. “In our clinic, having this team approach allows us to manage each child’s condition holistically, which is especially important since there is no specific treatment for long COVID.”
In Lucas’s case, he was first seen by an infectious disease physician who assessed his symptoms and spoke with the family to identify the symptoms that were most disruptive to his quality of life. Lucas, who had been suffering from chronic, painful headaches, received a referral to CHLA’s Neurological Institute where he was evaluated by a neurologist who recommended multiple options to manage the migraines. By November 2021, more than two months after his initial COVID-19 diagnosis, Lucas started to finally feel back to normal.
Understanding the mystery of long COVID
One of the most frustrating parts about long COVID is just how little is known about the condition: how many children and teens have it, why it impacts certain kids and not others, and whether it will affect their health in the future.
Researchers at Children’s Hospital Los Angeles are focused on answering these questions. CHLA is one of 10 pediatric centers across the country participating in a study called RECOVER (Researching COVID to Enhance Recovery) to delve into the mystery surrounding the aftereffects of a COVID-19 infection in the pediatric population. Currently, most information about long COVID is based on the experience of adult patients.
The goal of RECOVER is to enroll 20,000 children and young adults under the age of 25 across the U.S., including people experiencing long-term effects of COVID, those who recovered completely from COVID and people who never had COVID, as well as their parents and caregivers.
“We really want to see how prevalent long COVID is out in the community, not just the patients who come to our clinic, because there are people who aren’t aware they have long COVID and are tying their symptoms to something else,” explains Dr. Mohandas, one of the Principal Investigators of the National Institutes for Health-funded RECOVER study. “Each child is different with their own story, and research allows us to piece all these stories together.
“A single patient can only provide so much information,” she adds. “Once we have a better, more comprehensive understanding, we can then work on finding some kind of intervention.”
Shedding light
Lucas and his parents, Robert and Lisa, saw the opportunity to enroll in the RECOVER study as their chance to give back. They hope their participation can contribute to the scientific community’s knowledge about long COVID to help other kids suffering from the condition.

“We feel fortunate that Children’s Hospital was able to see Lucas quickly because it was a scary time,” says Robert. “He would ask us, ‘Is this how I’m going to be forever?’ And I didn’t know what to tell him. Not knowing the answers felt like I was letting my son down.
“I know there are other families out there like us, which is why I think this study is so important,” he adds.
Today, Lucas is doing well—back at school and maintaining a 4.0 GPA. His long COVID symptoms have nearly disappeared. He still experiences sporadic moments of nausea about once a month but “that is way better than when I was nauseous every hour and every day,” he says.
And like his parents, Lucas is also optimistic the RECOVER study will be beneficial.
“I hope it will shed some light, give us answers and lead to better treatments in the future,” he says. “If I can help be a part of that, that would be a blessing.”
Click here to find out more information about the RECOVER study at Children’s Hospital Los Angeles.



