New Test Could Transform Shunt Failure Diagnosis in Hydrocephalus
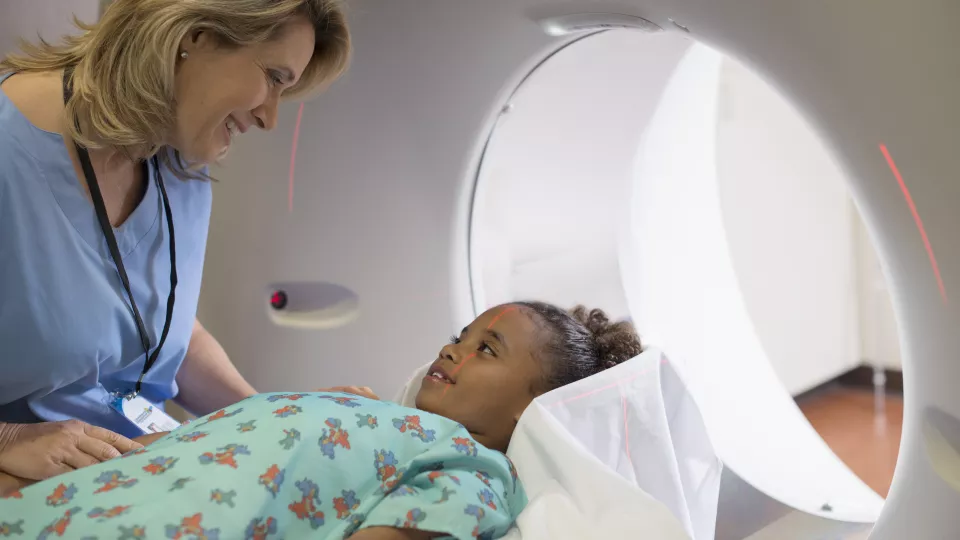
A Children’s Hospital Los Angeles team has developed a 60-second MRI test that may help to more easily diagnose shunt failure in children with hydrocephalus—a condition in which cerebrospinal fluid (CSF) builds up in the brain.
The noninvasive test, which uses phase-contrast MRI, is the first to precisely measure a key factor: how much fluid is flowing through a child’s shunt. Flow through a shunt is the primary metric for how well a shunt is working, so when flow starts to decline, this indicates the shunt is beginning to fail. The test is already being incorporated into clinical use at CHLA.
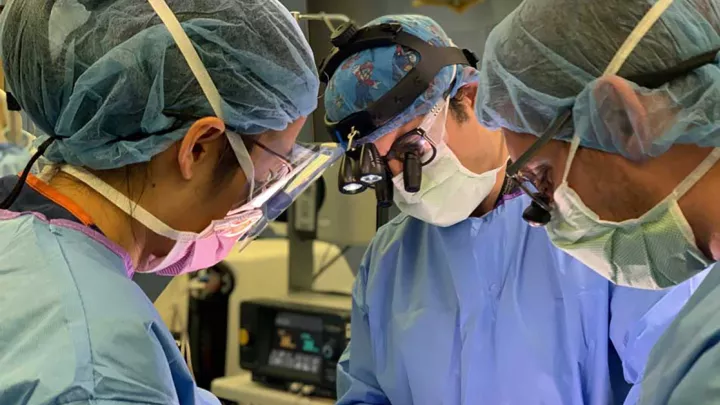
Peter Chiarelli, MD, DPhil, a pediatric neurosurgeon in the Neurological Institute, led the groundbreaking study, which was published in the Journal of Neurosurgery and involved multiple collaborators, including Chief Emeritus of Neurosurgery J. Gordon McComb, MD, as well as investigators Stefan Bluml, PhD, and Matthew Borzage, PhD. Recently, he also presented results at the 2023 American Association of Neurological Surgeons/Congress of Neurological Surgeons Joint Section on Pediatric Neurological Surgery conference—which earned him the Hydrocephalus Association Award.
Dr. Chiarelli shares how this test will improve patient care and accelerate opportunities for research.
Why is this test needed?
Shunts are lifesaving devices. But when your child has one, you live under the constant shadow of the possibility that that shunt will fail. Because if that happens, it can be life-threatening. And it does happen.
Unfortunately, we don’t have a test that can definitively diagnose shunt failure. We do a variety of tests, such as an MRI to see if the brain’s ventricles are enlarged. We’ll do a shunt tap. We may do a nuclear medicine study.
Many of these tests are invasive or painful or involve radiation. And yet, none of them tell us what we really want to know, which is: Exactly how much fluid is flowing through the shunt? That’s the Holy Grail. And that’s what this new MRI sequence does—it gives us that number.
How did this study come about?
We put together a research team called the CSF Flow Dynamics Group, which includes neurosurgeons, radiologists, biomedical engineers, and MRI physicists at CHLA. We work on different projects, but our initial idea was this one: Can we use MRI to measure how well a shunt is working?
Our goal is to find simple ways to solve major clinical problems right now, using technology that is available today. In this case, phase-contrast MRI is well established. We created a sequence that would work for this specific application, and then tested and validated it.
Has it changed your clinical practice?
We’ve been transitioning this test into routine clinical care at Children’s Hospital Los Angeles. Every child who comes in with a question of shunt failure gets this test. Our neurosurgeons are now looking for these numbers as we manage patients.
The nice thing is, it’s not an extra test. These children would already get an MRI anyway. It just makes that MRI one minute longer.
I see this as a valuable adjunct to standard care. We’re still doing things like shunt taps because that is the clinical standard, and we want to be as rigorous as possible. But I do see this MRI as potentially replacing a nuclear medicine test.
How will this impact patient care?
At CHLA, we see on average one to three patients each day where we’re evaluating for possible shunt failure. This same scenario is happening at centers across the country, which is one reason this test has the potential to be so impactful.
More accurately diagnosing shunt failure would give families peace of mind and prevent neurosurgeons from having to do nuclear medicine tests or unnecessary surgeries. It could also allow surgeons to diagnose shunt problems sooner—before they become emergencies for kids and their families.
What happens next?
We want to study this as part of a national, multicenter clinical trial. Our initial research was in 21 patients; we’ve since acquired data on over 200 children. We have received funding, and are applying for additional grants to support that trial, and we’re in the process of writing a paper on additional novel findings from our data.
Our team is also conducting clinical studies to help us better understand how certain factors—like eating or exercise—affect CSF production.
What does this mean for future research?
It’s exciting because this test gives us a new avenue for investigating basic shunt flow physiology.
So now we can study things like: What flow values are better for kids? Should we design a better shunt to optimize that flow? And even: Do certain patients not need their shunts anymore? Those are questions we haven’t been able to study in the past. But all of a sudden, we have a test. It opens up a whole new world.
Study authors were Joseph H. Ha, Matthew T. Borzage, Erik B. Vanstrum, Jacob K. Al-Husseini, Eamon K. Doyle, Meenakshi Upreti, Benita Tamrazi, Marvin Nelson, Stefan Blüml, Malkiat S. Johal, J. Gordon McComb, Jason Chu, Susan Durham, Mark Krieger, Rex A. Moats and Peter A. Chiarelli.