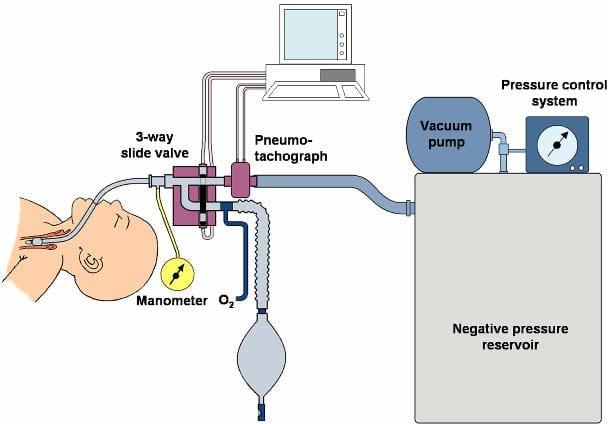
Our primary research interest is the development of new pulmonary function techniques appropriate to pediatric patients, utilizing specific equipment along with the personal computer to establish the safety of these methods and to determine the normal values, as well as the profiles of abnormality in various lung diseases. In addition, the response of the pulmonary system to therapies and the suitability of certain types of pulmonary abnormalities to new types of ventilation are also being evaluated.
Several other studies are concurrently being conducted within the national Collaborative Pediatric Critical Care Research Network (CPCCRN), funded by the Eunice Kennedy Shriver National Institute of Child Health and Human Development, some of which are listed below. The Network seeks to reduce morbidity and mortality in pediatric critical care illness and injury by developing an infrastructure to pursue well-designed collaborative clinical trials and meaningful descriptive studies in pediatric critical care. It is currently comprised of seven clinical trial centers, plus a data coordinating center, and is in its second grant cycle.
There have been a number of publications in several peer-reviewed journals as a result of the collaborative efforts of participating sites. Each center has its own principal investigator (PI) and is responsible for developing new research protocols and training procedures, monitoring conduct of Network studies and data collection, and ensuring adherence to quality assurance measures. I am the PI of the Network Center that includes Children’s Hospital Los Angeles and Mattel Children’s Hospital at the University of California Los Angeles. For more information about the Network, including completed and ongoing projects, visit http://cpccrn.org.
Current Funding
Ongoing studies currently funded by the National Institutes of Health in the form of U10, U01 and R21 grants:
1. Collaborative Pediatric Critical Care Research Network
U10 Grant: $296,416 per year for 10 years from 2005
The goal is to develop an infrastructure to pursue certain pediatric critical care medicine studies in order to reduce morbidity and mortality in pediatric critical illness and injury and to provide a framework for the development of the scientific basis of pediatric critical care. A sampling of studies being conducted:
- Critical Asthma - An analysis of the management, morbidity and mortality of severely ill children with asthma admitted to the PCIUs across the United States, with a view to planning prospective interventional trials.
- Critical Pertussis - A prospective cohort study evaluating morbidity, sequelae and mortality of children with pertussis.
- Bereavement Studies - Studies designed to develop an evidence-based framework for physician-parent follow-up meetings and to investigate the effect of these meetings on parental bereavement outcomes.
- Trichotomous Outcome Prediction in Critical Care - Prospective observational study to derive and validate a predictor of three or more outcome states following pediatric intensive care.
2. Therapeutic Hypothermia after Pediatric Cardiac Arrest Trials
U01 Grant: $22,118 per year for five years from 2009
A large multi-center randomized controlled trial examining effects of therapeutic hypothermia versus normothermia after pediatric cardiac arrest.
3. Translating an Adult Ventilator Computer Protocol to Pediatric Critical Care
R21 Grant: $224,936 over two years from 2010
A multi-center study designed to translate a developed adult computer-based decision support tool for management of Acute Respiratory Distress Syndrome to pediatric critical care.

