Bridging a Neonate With a Single Ventricle to Heart Transplant
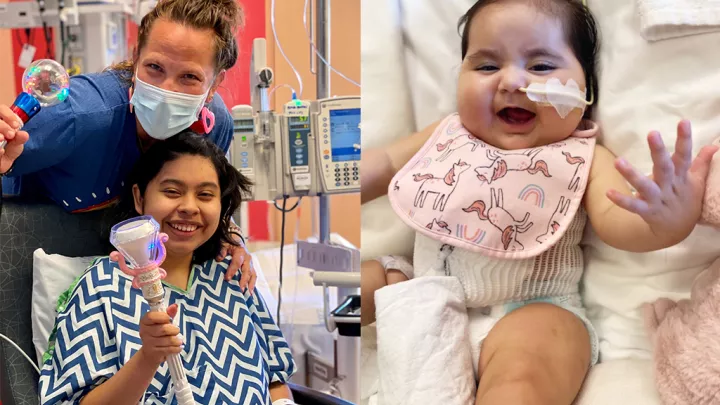
In a rare and high-risk procedure, a 1-month-old baby became the first patient with single-ventricle heart disease to receive a ventricular assist device (VAD) at Children’s Hospital Los Angeles.
The baby, who went on to receive a successful heart transplant, spent six months on mechanical support at CHLA in 2022—first on a PediMag device, followed by the Berlin Heart. The child is now 1 year old and doing well.
Surgeon John Cleveland, MD, who implanted the VAD and later performed the baby’s transplant, and Jennifer Su, MD, Director of the Ventricular Assist Device Program at Children’s Hospital Los Angeles, discuss this milestone procedure, the innovative way the VAD was connected—and the future of VADs in these high-risk patients.

How rare is it for a neonate with single-ventricle heart disease to receive a VAD?
Dr. Cleveland: It’s pretty rare. Only a few centers are doing these procedures in patients with single-ventricle disease, and in neonates it’s particularly unusual. In this case, the baby was only 3.2 kilograms when we put in the VAD.
In the past, our program had been reluctant to offer VADs for these patients because of the substantial risks. Nationally, only 30% of patients in their first stage of palliation end up surviving to transplant with a VAD. The odds are really stacked against them.
Talk about this case. Why was a VAD the only option?
Dr. Su: The baby came to our hospital at 1 week of age and was diagnosed with pulmonary atresia with intact ventricular septum—with a severely underdeveloped right side of the heart—as well as left ventricular noncompaction, a type of cardiomyopathy.
Because the baby was too unstable for surgery, we performed a patent ductus arteriosus (PDA) stent procedure in the Cardiac Catheterization Lab to try to improve blood flow to the lungs. But the patient remained unstable and later spent a week on extracorporeal membrane oxygenation (ECMO).
Dr. Cleveland: At that point it was clear the patient was in acute heart failure and would not survive to transplant without mechanical support. With the whole team on board, including the patient’s amazing family, we implanted the VAD just one day after the baby came off of ECMO.
You took a unique approach in connecting the VAD. What happened?
Dr. Cleveland: VADs need blood to flow into them to work. Because of this patient’s unique anatomy, we needed to take a different approach to ensure that the cannulas didn’t get blocked and that they had access to as much blood as possible.
To do this, I reversed the utility of the cannulas, which are the tubes that connect the VAD to the heart. I placed the aortic cannula on the atrium instead of the aorta—so instead of delivering blood to the body, it took it from the body back to the VAD. Then I took the cannula that we normally put in the ventricle and put it on the aorta to send blood to the body.
Why did you start with a PediMag?
Dr. Cleveland: In first-stage palliated disease, you’re asking a VAD to supply blood flow to both the body and the lungs. The PediMag is a magnetically levitated pump, and you can dial it up and down much more easily than with the Berlin Heart. That allowed us to make continual adjustments until we found the optimal cardiac output levels.
Dr. Su: After 2 ½ months, we switched the patient to the Berlin Heart because it’s designed for longer-term use. The PediMag was still working well, but we wanted to make the change before any complications occurred. We did this right at the bedside, and it went very smoothly. Three months later, the patient received a new heart.

How do you see the future of VADs for children with single ventricles?
Dr. Su: We’ve already performed our second single-ventricle VAD in another child who is a little older. We were able to make quick decisions based on our previous experience. Children with single ventricles often have limited options for mechanical support while awaiting heart transplant, and innovative VAD strategies allow us to buy more time as they wait for a new heart.
Dr. Cleveland: While we’re beginning to have some success with VADs in this population, mortality remains extremely high. My own research is focused on finding a viable alternative to VADs for these patients. My hope is that eventually we will have a better option to bridge these children, but we’re not there yet.
What was most rewarding for you about this experience?
Dr. Su: It’s been exciting to see such a positive outcome for this child. In the past, this option was simply not available for babies like this. To see this patient make it to a successful transplant and thrive with a new heart has been really rewarding.
Dr. Cleveland: I’m incredibly proud of the entire team. Everyone had to constantly be in tune to what the patient’s body was saying it needed, so we could make the necessary adjustments. This child’s life is a testament to the dedication and expertise of countless people across our Heart Institute. It is a moment to celebrate.