COVID-19 Testing and Kids: Everything Parents Should Know

In the fight against COVID-19, we have several tools to stay safe and protect others. Vaccines help our bodies develop a robust immune response against infection, masks prevent the virus from spreading to others and continuing to practice social distancing and good hygiene habits can keep us healthy.
Another vital resource: testing. Even if you and your child are up to date on your COVID-19 vaccinations, experts still say it’s important to get tested, especially if you are feeling symptoms or have been exposed to someone who is sick.
“Testing remains one of the most crucial tools in our efforts to identify COVID-19 cases and control the spread of the virus,” says Jennifer Dien Bard, PhD D(ABMM), Director of the Clinical Microbiology and Virology Laboratory at Children’s Hospital Los Angeles. “Additionally, testing is also key to our understanding of the genetic makeup of the virus and to identifying important mutations.”
What’s the best kind of test for children? And when should they be tested? Here’s everything parents need to know about testing kids for COVID-19, according to Dr. Dien Bard.
Choosing the right test for your child
There are two main types of COVID-19 tests available that can tell whether you are currently infected with SARS-CoV-2, the virus that causes COVID-19:
- A molecular test, also called a nucleic acid amplification test (NAAT), detects genetic material within the COVID-19 virus. The majority of samples must be analyzed in a laboratory. Polymerase chain reaction (PCR) tests are one of the most common NAATs.
Pros:
- Highly accurate
- Considered the “gold standard” of COVID testing
- Can identify positive cases even if the patient is infected with a variant, such as Delta or Omicron
- More sensitive and specific than antigen tests
Cons:
- Results may be typically available within hours or days, depending on the services offered by the clinical laboratory
- An antigen test detects proteins on the surface of the COVID-19 virus.
Pros:
- Results are faster than molecular tests, usually within 30 minutes or less
- Convenient and at-home test kits are available
Cons:
- Not as reliable as molecular tests in identifying true positives and true negatives
If your child has to be tested to meet certain requirements for school, sports leagues, travel or another activity, be sure to check which test is required.
Diagnostic tests vs. antibody tests
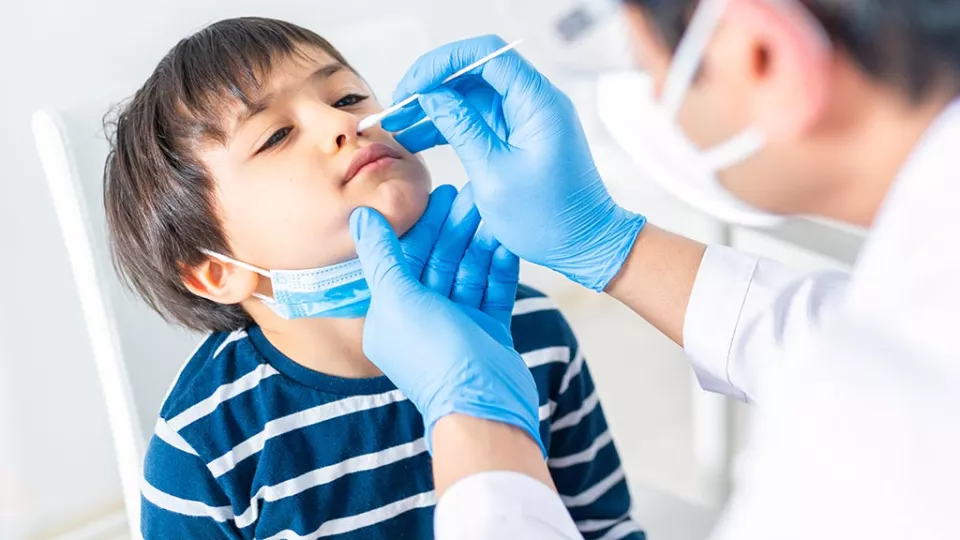
Molecular and antigen tests are diagnostic tests that detect a current infection. Samples are taken using saliva or a swab from the nose or throat.
An antibody test, also called serology, cannot tell if your child currently has COVID-19. Instead, it checks for antibodies made by the immune system to see if there was a COVID-19 infection in the past, and some tests can also detect if you have antibodies as a result of being vaccinated. Samples are taken from a blood draw, either in the arm or through a finger stick.
The difference between a nasal swab, throat swab and saliva test
The gold standard to test for SARS-CoV-2 is a nasopharyngeal swab (NPS). Collecting a sample this way must be performed by a trained health care worker and can often be uncomfortable. Other types of nasal swabs include mid-turbinate swab (MTS) and anterior nares swab (ANS), which are collected inside the nose without going as deep as an NPS and are less uncomfortable.
Saliva has been proven to be a promising specimen for detecting SARS-CoV-2 as well. For saliva tests at Children’s Hospital Los Angeles, we provide a small tube that patients can directly spit into and request at least 3 milliliters of saliva to increase the chances of detecting the virus.
Throat swabs can also be collected, but can be less sensitive. Studies have found that having a throat swab plus an ANS tested together can perform just as well as an NPS or saliva sample.
How accurate are the different kinds of tests?
PCR tests are ultimately the gold standard for testing. They are highly accurate and the most sensitive compared to any other tests available to the public. One downside of PCR testing is that the sample has to be sent to a laboratory for analysis, and results can take longer, especially if the laboratory is overwhelmed with specimens.
An alternative to PCR tests is antigen testing, which is very fast and can offer results in 10 to 20 minutes. There are also at-home antigen test kits available, which makes antigen testing very convenient. A major limitation, however, is that it is not very sensitive—and a negative result does not always mean you don’t have COVID. For example, if someone tests negative using an antigen test but is symptomatic, Dr. Dien Bard highly recommends a PCR test or repeating an antigen test the next day, if possible. In the meantime, you should still assume they have COVID and isolate.
When to get tested
For both PCR and antigen tests, the timing of testing is important, says Dr. Dien Bard. If your child has been exposed to someone with COVID, and you decide to get a PCR test, have them tested three to five days after the exposure. Testing too early (e.g., one day after exposure) can lead to a false negative result.
Because PCR tests are more sensitive, the window of testing is larger compared to antigen testing. A child can test positive on day 3 with a PCR test; with an antigen test, that same child may not be positive until day 5 or 6.
An antigen test’s accuracy is also dependent on how prevalent cases are during the time of testing. During the surge of the Omicron variant, when rates were high, a positive antigen test could be trusted without the need for a PCR test. However, when cases are low, a positive antigen test—particularly for an asymptomatic child—should be confirmed with additional testing to ensure the result is not a false positive.
Consider getting a COVID test if your child:
- Is experiencing COVID-19 symptoms, even if they are vaccinated or has had COVID-19 in the past
- Has been in close contact with someone who had COVID-19 within the last 10 days
- Is attending an indoor gathering or event, particularly if other attendees’ vaccination status is unknown or if there will be people who are considered high risk for severe COVID-19 illness
- Is planning to travel; according to the Los Angeles County Department of Public Health:
- For domestic travel, get tested 1 to 3 days before travel and 3 to 5 days after returning home.
- For international travel, testing may be required before and after arriving in other countries, and is required for returning to the U.S.
- Is attending school and isn’t fully vaccinated
Home testing vs. testing at a facility (hospital, doctor’s office, testing site, etc.)
If your child is symptomatic, parents can use an at-home antigen test. If it shows a positive result, the test can be trusted, and your child should isolate from the rest of the household, according to Dr. Dien Bard. If the antigen test is negative, however, consider going to a testing site or doctor’s office to get a PCR test, which is more sensitive. Isolate the child in the meantime until the PCR test result comes back.
What to do if your child tests positive for COVID-19
Contact your pediatrician or health care provider and notify your child’s school. Your will need to follow the school’s instructions for isolation and when your child can return. In the meantime, your child should not attend class, socialize or participate in in-person activities like sports. Keep the child isolated from anyone outside the family. If possible, designate one vaccinated adult caretaker to be with the child and wear medical grade masks whenever possible.