Arteries are alive. They carry blood to the body’s cells, but they’re made of living cells themselves. If the body is injured in some way, arterial cells immediately respond at the site of injury. They grow and divide and make new pathways to bring blood where it is needed to heal. Normally this process is tightly controlled, and the arteries get smaller and smaller until they become capillaries and then veins.
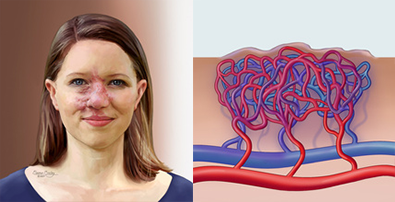
In an arteriovenous malformation (AVM), the control of this process breaks down. When arterial cells lose the ability to turn off their growth, they keep making new pathways that the body doesn’t need and doesn’t want. These pathways don’t work like they’re supposed to and lack the microscopic capillaries that supply the body’s cells. Instead, an arteriovenous malformation is a direct connection between artery and vein, and any blood that passes through it goes back to the heart without doing anything useful along the way. This can lead to a number of problems and symptoms.
Many patients with an arteriovenous malformation may have subtle symptoms at first: increased pulsatility or vibration (known as a thrill) at the site of the AVM; skin changes like discoloration or increased warmth; pain with activity or at rest. Over time, the increased blood flow through an AVM can lead to overgrowth of the affected body part. If left untreated, severe cases of arteriovenous malformation can cause bleeding, tissue loss or heart failure.
Diagnosis
You/your child will meet with the Vascular Anomalies Center team during the initial clinic visit for a comprehensive review of the patient’s medical history, any imaging studies and/or laboratory tests that have been performed, and a complete physical examination. The medical specialists will then confer and diagnose the condition and propose a treatment plan.
Additional testing may include:
- Ultrasound
- MRI
- Diagnostic angiography
- Genetic testing
Treatment
Treatment is individually tailored to the particular arteriovenous malformation in question. Small lesions in safely-accessible areas may be surgically removed. The mainstay of treatment, however, is endovascular embolization, a minimally-invasive procedure where a physician goes into the AVM and then blocks the areas of blood flow. This is typically done in a step-wise fashion, as the cells of an arteriovenous malformation are prone to over-active healing, and multiple sessions of therapy are the standard. Endovascular embolization is almost always an outpatient procedure, and the expectation is usually to return to school or work the following day.
