Brachial Plexus and Peripheral Nerve Program
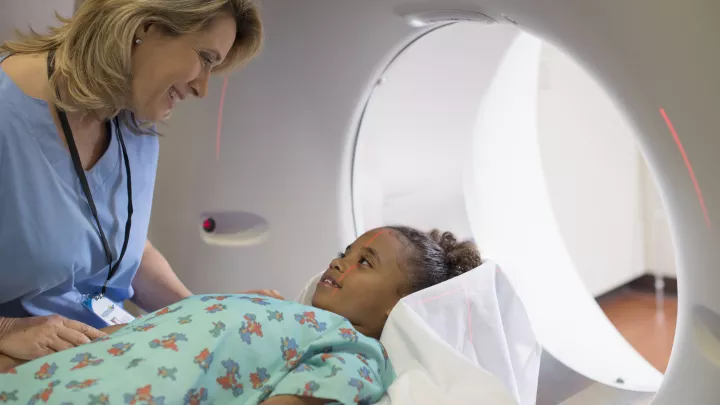
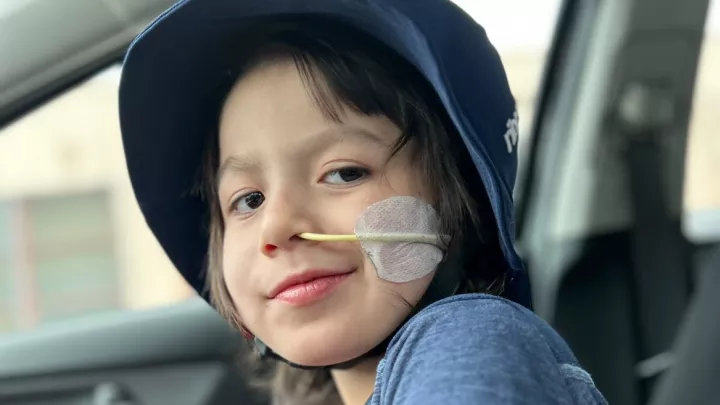
Children’s Hospital Los Angeles is home to the West Coast’s largest Brachial Plexus and Peripheral Nerve Program. A brachial plexus or peripheral injury affects nerves that lead from the spinal cord to the rest of the body. These injuries can lead to a loss of limb sensation or movement.
Our program brings together experts from our nationally ranked Neurological Institute and Jackie and Gene Autry Orthopedic Center. Our program sees far more patients and performs more complex brachial plexus and peripheral nerve surgeries than most other pediatric centers in the country. This experience caring for a large number of children is just one reason why we achieve exceptional results. We offer help and hope to your family.
What Are Brachial Plexus and Peripheral Nerve Injuries?
Peripheral nerves are a network of nerves connecting the brain and spinal cord to the upper and lower limbs. Injuries to these nerves can lead to a loss of limb sensation or movement.
Brachial plexus and peripheral nerve injuries may occur:
- During childbirth, if the nerves are stretched or torn
- Accidentally from sports injuries, car accidents, falls or other trauma
- As the result of a virus, tumor or cancer treatment, such as radiation therapy
- Without known cause or injury
Brachial Plexus and Peripheral Nerve Conditions We Treat
Experts at Children’s Hospital treat the full spectrum of brachial plexus and peripheral nerve conditions, including:
- Brachial plexus injuries: These injuries affect the bundle of nerves (brachial plexus) in the neck that control movement and sensation in the shoulder, arm and hand.
- Peripheral nerve injuries: Damage to peripheral nerves affect the body’s ability to send signals from the spinal cord to the rest of the body.
- Nerve palsies: Compression or injury to a peripheral nerve can cause pain, numbness or weakness in the arm or leg. These may include:
- Common peroneal palsy: This causes numbness along the outer leg and the top of the foot. It can lead to a problem known as foot drop.
- Median and ulnar nerve palsies: These can cause pain, hand weakness and difficulty with fine motor control of the hand. They can also cause numbness throughout the hand.
- Tumors of the peripheral nerves (nerve sheath tumors): Tumors can occur on the nerves themselves and can cause pain, weakness or loss of feeling in the arm or leg.
Brachial Plexus and Peripheral Nerve Care: Why Choose Us
Children’s Hospital is home to one of the most comprehensive programs of its kind in the country. Our program brings together all of the experts your child needs.
We offer:
- Team approach to care: Nerves, muscles and bones work together, which is why your child’s care team includes leading experts in these fields. Our pediatric specialists coordinate services to effectively help your child regain sensation and movement. Our surgeons perform more complex peripheral nerve surgeries on infants and children than almost anyone in the country. Meet our doctors.
- Range of treatments: Some injuries improve without surgery. If your child needs surgery, we offer the most advanced brachial plexus and peripheral nerve injury treatments. Our doctors are among an elite few in the country with the expertise to move nerves from one muscle to another (called a nerve transplant) to restore sensation and movement to the affected limb.
- Focus on noninvasive treatments: Our occupational therapists have advanced training in helping children with brachial plexus and peripheral nerve injuries. Some children get better with therapy alone. Others benefit from therapy before and after surgery.
- Care for complex injuries: If your family was told that surgery isn’t an option for your child—or a previous surgery didn’t achieve the desired outcomes—we have the expertise to help. We offer advanced brachial plexus and peripheral nerve injury treatments from diagnosis to many years later.
- Advanced diagnostics: Children’s Hospital is one of a few centers in Los Angeles that offers electromyography (EMG) and nerve conduction tests for children. These tests assess muscle and nerve function. This information helps our surgeons develop the best treatment plan.
- Support for your family: The CATCH Hand Differences Program offers activities and services for children and families, including an annual Handy Heroes Therapy Camp.
Our Team Approach to Brachial Plexus and Peripheral Nerve Injuries
Children’s Hospital takes a unique team approach to treatment, especially surgeries. A neurosurgeon and an orthopedic surgeon perform your child’s procedure together. They address every issue together during surgery, giving your child a better chance at regaining movement and function.
Your child’s care team includes:
- A neurologist, who conducts diagnostic tests to identify nerve and muscle injuries
- A neurosurgeon, who is specially trained to perform surgeries on nerves
- An orthopedic surgeon specially trained to perform surgeries on nerves
- Occupational therapists who perform stretching and movement exercises that are important both before and after surgery.
Specialized Clinic for Brachial Plexus and Peripheral Nerve Injuries
At our specialized clinic in the Neurological Institute, your child sees multiple specialists during the same appointment. This makes care more convenient for your family.
Second Opinions for Brachial Plexus and Peripheral Nerve Injuries
When your child has brachial plexus or peripheral nerve injury symptoms, an accurate diagnosis is essential. This information enables doctors to deliver timely, appropriate care. Our experts regularly provide second opinions and treatment recommendations. You do not need to live in the Los Angeles area to benefit from these services.
Request a second opinion from Children’s Hospital Los Angeles
To schedule an appointment for a second opinion neurological evaluation, please call 323-361-2471. You may also request an online second opinion.