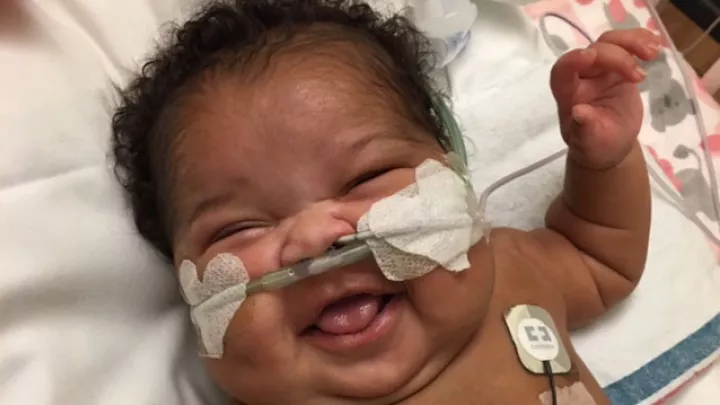
Small but Mighty: Courageous Kennedy Grows Stronger
Kennedy Rae Lewis’ mom expected her first ride to be in the back seat of her car on the way home from the hospital. Instead, it was in a helicopter, just hours after she was born—and it was a ride on which her life depended.
Kennedy arrived ten weeks early via emergency cesarean section due to complications in the womb. As doctors at an adult hospital in Antelope Valley were assessing Kennedy’s lack of fetal movement, her heartbeat stopped.
“I was terrified,” says Kennedy’s mother, Marrietta Lanier, “… to think that your baby could one minute be moving inside of you and then the next, not be.”
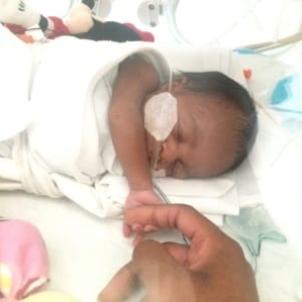
Once Kennedy was out of the womb, the trouble didn’t stop there. Kennedy not only had to overcome problems with prematurity such as breathing issues, immature skin and growth issues—but also birth defects. She was diagnosed with VACTERL association; each letter of the acronym represents a rare birth abnormality, and she suffered from three of the six. Doctors discovered that her esophagus was not connected to her stomach, and that she had no opening at the end of her digestive tract. There were other complications with her genital and urinary organs as well. Realizing she needed more specialized care, doctors had to transfer her to a place that could adequately care for a fragile newborn like Kennedy.
“I had a few options, but I immediately chose Children’s Hospital Los Angeles,” says Marrietta. “This is a place for children, so why wouldn’t I want this to be the place for her?”
Kennedy’s fight
Kennedy’s extreme situation required her to be flown to CHLA’s Steven & Alexandra Cohen Foundation Newborn and Infant Critical Care Unit (NICCU) four hours after she was born—and without mom by her side. “I couldn’t hold her right away and that was the worst for me,” says Marrietta. “When your child comes out, that’s what you want to do and bond with them, but I couldn’t.”
The next day, surgery was scheduled with Tracy Grikscheit, MD, a pediatric surgeon at CHLA, to determine how best to support the issues with her digestive system and provide her with nutrition so she could grow.
“When Kennedy first came to us, she was very small … and her lungs were premature, which makes any surgery high-risk,” says Rachel Chapman, MD, medical director of the NICCU and one of the many medical experts on Kennedy’s case.
During the first surgery, the surgeon discovered that her esophagus gap was very long—making her case more challenging than the doctors had thought. Kennedy would have to wait as CHLA specialists worked to support her growth, allow her lungs to become healthier, and bring the two ends of her esophagus and stomach closer together.
A mother’s love
With her daughter in the operating room at Children’s Hospital, Marrietta was still at her own local hospital, receiving updates from Kennedy’s care team. Fighting the medication that made her drowsy, Marrietta made her way to Kennedy’s side just 24 hours after giving birth.
When a child is admitted to CHLA, members of the medical staff sit down with the family to let them know who will be involved in their child’s care, what the major complications may be, what steps need to happen quickly, what the care team’s focus will be and what the health goals are both short- and long-term. The staff also encourage parents to be involved in their child’s care.
“Marietta has been very present, and it has been beneficial to Kennedy in terms of both maximizing her development and making mom a partner in her care,” says Chapman.
The CHLA support team
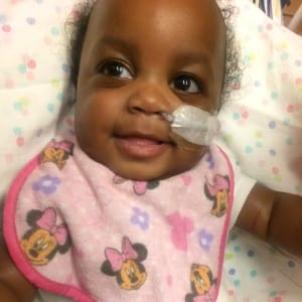
In cases as complex as Kennedy’s, CHLA assembles a multidisciplinary care team, which includes a neonatologist, a nurse practitioner, a pediatric resident, neonatal nursing staff and specialists in respiratory services. Kennedy’s team also includes pediatric specialists in general surgery, urology, pulmonology and nephrology.
CHLA is also able to support Kennedy’s development while she’s in the hospital and help minimize some possible setbacks through physical, occupational and feeding therapy, music therapy, reading programs and the help of Child Life specialists.
“She’s learning to roll over and sit up,” says Marrietta. “Throughout this whole process, I wasn’t sure how my baby would turn out. But to see her developing normally … it’s comforting.”
So far, Kennedy has gained 11 pounds and is almost ready for the surgery that will connect her digestive organs together and address the issues that she has with her urological system.
Kennedy has already gone through many adversities. But despite this, she’s a happy baby who loves music, smiling and tickles from mom. Kennedy has lived up to the name Marrietta chose for her: “It’s the name of a warrior. I wanted her to be strong and have a strong name that she could grow with.”
Where Kennedy is now
Kennedy, who is now 1, has found a love for books. In fact, she loves books so much that she has 365 of them! And that’s mostly due to the hospital’s Literally Healing Program, which provides patients with one new book every day they’re in the hospital. That means Kennedy has now spent a full year in the NICCU at Children’s Hospital Los Angeles.
In the past year, she has made great strides with her medical prognosis. Last November, she was able to finally receive esophageal repair surgery—the biggest surgery she was waiting for, to connect her esophagus to her stomach. She also received vaginal plasty and fixes to her uterus.
Kennedy has also progressed well developmentally. She loves playing with her favorite toy: a piano that lights up. She now stands up on her own, is starting to walk, is learning how to talk and has a full mouth of teeth.
“For all that she’s gone through, she is handling everything really well,” says Marietta. “She is just like any happy baby.”
Kennedy got to go home for the first time in June, but she is now back in the hospital, and will most likely have years more of treatment. Currently, the next steps are to get her off of a colostomy bag and build up her immune system.
“There are a lot of things that can put her down, like a fever,” says Marietta. “But nothing can keep her down for too long. She is resilient.”